Oral Facial Surgery Center
How to Take Care of Your Dental Implants
 Cleaning and taking care of your implant is just as important as cleaning your natural teeth. Here are some things you should know about caring for your implant.
Cleaning and taking care of your implant is just as important as cleaning your natural teeth. Here are some things you should know about caring for your implant.
Your implant and your natural teeth are similar because they both rely on healthy tissue for support and both can build up plaque. It’s important to remove that plaque because it can develop into an infection. If the infection isn’t properly treated, it can result in a loss of bone around the implant which could progress to the loss of the implant itself.
It’s important to get your teeth cleaned on a regular basis so your dental hygienist can get that biofilm off your teeth and keep your teeth infection-free. As always, you should be brushing your teeth and flossing twice a day. Never use your teeth, especially your implant as “scissors” to open anything.
Dental implants are the closest thing you can get to real and natural teeth. They don’t require any special products or treatment. Just a simple brush and floss will do the job. They are also long lasting. If they are properly cared for, they can last a lifetime, avoiding any further dental work down the road.
With a dental implant, you can still enjoy all your favorite foods. It will not loosen or fall out if you are chewing something hard.
Overall, dental implants are meant to make life better and easier, not to add issues or interrupt your life. You don’t have to go out of your way to take care of them – a simple brush and floss will ensure that they improve your overall quality of life for many years to come.
If you think a dental implant may be right for you, call Oral Facial Surgery Center at 985-879-1972 to schedule a consultation with us.
Posted by
tguidry
on
Oct 2nd, 2017
6:48 am
Posted in
Blog, Dental Implants |
Comments Off on How to Take Care of Your Dental Implants
Better Breakfast for a Better Smile
Breakfast truly is the most important meal of the day. It kick starts your body and provides you with enough energy to make it through your hectic morning as well as keep your mind focused on the task at hand. Eating a balanced breakfast is not only good for you body, but also good for your teeth. Being mindful of the acidity and sugar levels in your food is key to keeping your teeth in tip-top shape!

When it comes to breakfast foods, there are a few foods we recommend eating in moderation! These include, but are not limited to, orange juice and sugary cereals. Orange juice has a very high acidity and by drinking too much, the acid can wear down your tooth enamel. Cereals that are high in sugar have a similar effect on your teeth, but the sugar can also cause cavities.
Eating a balanced breakfast that is low in sugar and acid, but high in protein will make your body and teeth feel great! Protein rich foods will help to build up your enamel and keep your teeth stronger than ever.
Here are a few recipe ideas for a healthy and balanced breakfast:
Overnight Oats:
o 1/3 cup of oats
o 1/3 cup of milk (or substitute almond, soy, coconut, etc.)
o 1/3 cup of plain Greek Yogurt
o 1 tbsp chia or flax seeds OR ¼ cup chopped nuts
o Fresh fruit/ berries of your choice!
Mix all of the ingredients together in a sealed container, or mason jar, and place in fridge the night before. Open and enjoy the next morning for a healthy and balanced breakfast!
Avocado Toast:
o 1-2 slices of whole grain toast
o 1 ripe avocado
o 1 egg (cooked to your preference)
o 1 ripe tomato
o Seasonings of your choice (salt & pepper, hot sauce, red pepper flakes, etc.)
Posted by
tguidry
on
Sep 10th, 2017
8:55 am
Posted in
Balanced Breakfast, Blog, Dental Health |
Comments Off on Better Breakfast for a Better Smile
Orthognathic Surgery
 What is orthognathic surgery?
What is orthognathic surgery?
Also known as corrective jaw surgery, patients undergo this procedure in order to correct a wide range of major and minor dental and skeletal irregularities. Jaw surgery is used to correct the misalignment of a person’s jaw or teeth, which will eventually improve breathing, chewing, and speaking. While a patient’s physical appearance may be altered just a bit with surgery, orthognathic surgery is mostly meant to correct functional problems.
What are some conditions that require orthognathic surgery?
There are quite a few conditions that indicate that you may need jaw surgery. Some of those include:
- Sleep Apnea (breathing problems during sleep)
- Protruding jaw
- Open bite (someone who is unable to fully close their mouth)
- Chronic mouth breathing and dry mouth
- Difficult biting food or chewing
- Difficulty swallowing
- Chronic joint or jaw pain (TMJ)
- Excessive wear on teeth
Evaluating Your Need For Jaw Surgery
We will work with your orthodontist and general dentist to evaluate your need for jaw surgery. In a great number of cases, patients need to have orthodontic work done before and after surgery. Jaw surgery is a lengthy and delicate process. In most cases, the whole process, including orthodontic work, will last 1-2 years. We will evaluate you thoroughly and realistically so that you may make the most informed decision possible.
How will I benefit from having jaw surgery?
Corrective jaw surgery will benefit you in numerous ways. After surgery, your jaw will be more aligned and balanced, and you will have more a far more functional and healthy jaw. While recovery may be lengthy, we will keep you comfortable along the way. With jaw surgery, patients can see an improvement in speech, eating, chewing and also breathing. Many patients see a positive change in their facial structures aw well after their jaw has been realigned.
To find out if you are a good candidate for corrective jaw surgery, please call us at Houma Office Phone Number 985-879-1972.
Posted by
tguidry
on
Sep 5th, 2017
8:46 am
Posted in
Blog, Jaw Surgery |
Comments Off on Orthognathic Surgery
New Trends in Dental Implants
 A trending topic right now seems to be the decision to opt for “mini-dental implants” instead of more traditional ones. Below we are going to take a look inside the trend, and lay out some of the benefits and drawbacks so that you can get a better understanding of this exciting trend in dentistry.
A trending topic right now seems to be the decision to opt for “mini-dental implants” instead of more traditional ones. Below we are going to take a look inside the trend, and lay out some of the benefits and drawbacks so that you can get a better understanding of this exciting trend in dentistry.
Benefits
- Mini dental implants are usually less expensive than traditional ones, sometimes costing only 1/3 that of regular implants. They take less time to place and are smaller and less invasive, and can be used in small spaces or for those with inadequate bone mass.
- With mini dentures, smaller dentures can be used, leading to a better tasting experience for the palate than a traditional denture would provide.
- Mini implants can be placed with minimal recovery time, and usually require very little to no bone grafting.
Drawbacks
Because this is still a fairly new procedure, there are a few downsides. For one, there aren’t enough studies out there on the longevity of these implants, so we don’t know how they hold up over time. A study published in the International Journal of Implant Dentistry in 2016 revealed that traditional dental implant placement has a proven survival rate of 95% or greater. The analysis collected data from over 10,000 implants from 3,095 patients, across three separate private practices over the course of 20 years. For mini dental implants, there isn’t yet enough data to conclude a proper survival rate.
Another concern is that because this is such a new trend there is not as much information or regulation out there. Some practices with claims such as “Dentures-in-a-day” might not do a proper consultation, skipping important steps such as a 3D scan to make sure that you are a good candidate for the procedure.
While it may be some time before this method is perfected and adopted, it is also exciting to see the advancements changing people’s lives in the dental industry every day. Check in with Oral Facial Surgery Center to find out what tooth replacement options may be right for you!
Posted by
tguidry
on
Aug 1st, 2017
8:41 am
Posted in
Blog, Dental Implants |
Comments Off on New Trends in Dental Implants
How to Make Your Own Ice Cream
 As you may or may not know, July is officially National Ice Cream Month! While it is fun to go and grab ice cream from your local shop down the street, it can be more fun and rewarding to make your own ice cream for you and your family to enjoy. Ice cream is also a great treat to enjoy after different types of oral surgery. You don’t need an ice cream maker in order to make delicious, creamy ice cream. Just follow our instructions below!
As you may or may not know, July is officially National Ice Cream Month! While it is fun to go and grab ice cream from your local shop down the street, it can be more fun and rewarding to make your own ice cream for you and your family to enjoy. Ice cream is also a great treat to enjoy after different types of oral surgery. You don’t need an ice cream maker in order to make delicious, creamy ice cream. Just follow our instructions below!
Servings: 2-3
Ingredients:
– 2 cups of milk
– 3 tablespoons of sugar
– 2 teaspoons of vanilla
Materials:
– 3-4 cups of ice
– 2/3 cup salt
– 1 quart sized Ziploc bag
– 1 gallon sized Ziploc freezer bag
Instructions:
– Combine milk, vanilla and sugar in quart sized bag
– Press any air out of bag and seal tightly
– Mix ice and salt in gallon sized bag
– Place quart sized bag into gallon sized bag and seal tightly
– Shake the bag vigorously for about 5 minutes.
– It will be very cold, be careful!
– Liquid inside smaller bag should start to harden
– Let bags sit for a few minutes with ice in large bag surrounding small bag
– Open bags up and scoop ice cream out
– Enjoy!!
As you can see, it isn’t hard to shake up some ice cream that the whole family can enjoy, using fairly standard household ingredients. Use chocolate/strawberry milk instead of regular milk to change the flavor, or use half and half for a creamier product. This year, celebrate National Ice Cream month by making your own ice cream at home!
Posted by
tguidry
on
Jul 14th, 2017
9:51 am
Posted in
Blog |
Comments Off on How to Make Your Own Ice Cream
Autograft vs. Allograft
 So, you were recently told by your doctor that you need a bone graft, but you aren’t quite sure what that means.
So, you were recently told by your doctor that you need a bone graft, but you aren’t quite sure what that means.
A bone graft is a surgical procedure that is used to fix bones or joints that were damaged by trauma, and it is also used to replace bone that is missing to provide structural stability around the body, including the jawbone. There are many types of bone grafts we can use to grow bone – the two most common are autografts and allografts.
An autograft is a bone or tissue that is transferred from one spot to another on the patient’s body. It is often thought of as the “gold standard” in bone grafting because of its reliability. Its high success rate is due to the fact that it is living tissue and thus its cells are kept intact.
An allograft is a bone or tissue that is transplanted from one person to another. They typically come from a donor, or cadaver bone. The allograft is safe, ready to use and available in large amounts. The main advantage of an allograft is that it requires one less procedure than the autograft, which must first be taken from the patient. Surgical time is minimized and the recovery can be quicker. The allograft comes from a reputable and reliable tissue bank.
Knowing which bone-grafting option you will need can be confusing, but we are here to answer any questions you may have. Please schedule a bone grafting consultation with us by calling Houma Office Phone Number 985-879-1972. We will perform a thorough evaluation of your oral health. After our evaluation, we will recommend what bone graft is best for you. We are happy to discuss your options and answer any questions you may have. We want you feeling confident with our choice and worry free.
Posted by
csaal
on
Jul 8th, 2017
8:49 am
Posted in
Blog, Bone Grafting |
Comments Off on Autograft vs. Allograft
Where Do Dental Implants Come From?
 Dental implants have a surprisingly rich and interesting history. Across centuries and throughout cultures around the world there is evidence of attempts at replacing missing teeth with various objects and materials.
Dental implants have a surprisingly rich and interesting history. Across centuries and throughout cultures around the world there is evidence of attempts at replacing missing teeth with various objects and materials.
The oldest dental implants can be traced back to 2000 BC in China, where missing teeth were substituted with bamboo pegs.
Fast forward a bit to around 1000 BC and you’ll find an ancient Egyptian King whose tomb was recently discovered along with his mummified remains; a copper peg hammered into place where a tooth once lived. This may have been the first time in history that we know of when metal implants were used.
Across the globe some time around 300 BC, an iron tooth was found in a French grave thought to be Celtic in origin. It is possible this implant may have been a post-mortem placement to honor the dead, as an attempt to perform the surgery using a live patient would have been an excruciatingly painful process.
Just 2000 years ago missing teeth were being substituted for animal teeth, and the poor were even selling their teeth to the wealthy, just to make ends meet! The body often rejected these surrogate teeth, causing infection.
More recently in 1931 in Honduras, Dr. Wilson Monroe and his wife found a jawbone amongst other artifacts, with teeth fashioned from shells and attached to the jawbone of an ancient man.
Today we are lucky enough to have dental implants that not only look and feel like real teeth, and anesthesia for the pain is also a plus. Thanks to studies conducted by Per-Ingvar Brånemark of Sweden in the 1950’s, oral surgeons have been able to perfect the process over the years to create today’s implants, which have a 98% success rate! Through a process known as osseointegration, metals and other implant materials are able to be skillfully placed so that your jaw bone actually attaches itself to the implant creating a seamless support system.
Missing a tooth or two? Give us a call at Houma Office Phone Number 985-879-1972 to discuss your dental implant options today!
Posted by
csaal
on
Jun 7th, 2017
8:48 am
Posted in
Blog, Dental Implants |
Comments Off on Where Do Dental Implants Come From?
Impacted
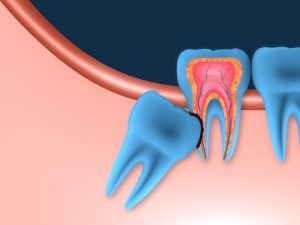 When you hear this word in our office, it is most likely that we are talking about your wisdom teeth. And while we know that it may sound scary to have “impacted wisdom teeth”, we want you to know that, actually, it is very common.
When you hear this word in our office, it is most likely that we are talking about your wisdom teeth. And while we know that it may sound scary to have “impacted wisdom teeth”, we want you to know that, actually, it is very common.
What are impacted wisdom teeth?
Throughout evolutionary history, human mouths (jaws) have become increasingly smaller. While the jaws have gotten smaller, the amount of teeth we have has not. So now we have the same amount of teeth squeezing into a smaller space. Because wisdom teeth are the last to erupt, they often become impacted – that is, blocked by the other teeth around them. Often they are growing in sideways or unable to erupt through the gums at all due to crowding.
Why do wisdom teeth need removal?
The inability to erupt properly means that wisdom teeth can cause a lot of pain and even become infected down the road. This is the main reason that we recommend the removal of all third molars (another name for wisdom teeth). The reason that we remove them during the teen years is that the bone is still soft and recovery from the surgery is taken by the patient much better at this age. If we were to wait, your teeth may become infected, your bite crooked, and it may be too late at some point for us to take them out.
Types of Impaction:
- Vertical Impaction – In this case, the tooth is unable to break through the gum line. Vertical impaction is very common.
- Mesioangular Impaction – Angled toward the front of the mouth, the tooth is probably pushing on its neighbor, causing pain and crowding. This type of impaction is also very common.
- Distoangular Impaction – This tooth is angled toward the rear of the mouth, it is uncommon.
- Horizontal Impaction – In this case, the tooth is a complete 90 degrees from where it should be, and is likely growing into the roots of its neighboring tooth. This is very rare.
What is the removal procedure like?
You will be completely pain-free during the surgery, which takes just about an hour. You will also be sent home with instructions for pain management, eating and rest orders.
What is recovery like?
You will recover comfortably at home. You can start drinking liquids and soft foods as soon as you feel ready, but should avoid crunchy foods, extra hot or cold items, and straws (NO STRAWS!). You can expect to resume some of your normal activities a few days post-operation.
If you have any questions about wisdom teeth removal or aren’t sure if you even need the procedure, give us a call at Houma Office Phone Number 985-879-1972!
Posted by
csaal
on
May 3rd, 2017
8:47 am
Posted in
Blog, Tooth Extraction, Wisdom Teeth |
Comments Off on Impacted
Preserving Your Jaw after Extraction: Socket Preservation
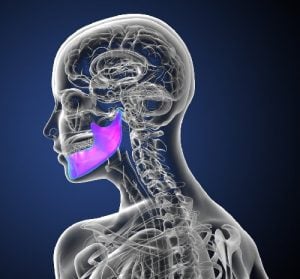 If you come to see us for an extraction, you may hear us talking about “socket preservation” or ”ridge augmentation”, and you might be wondering, what is that?
If you come to see us for an extraction, you may hear us talking about “socket preservation” or ”ridge augmentation”, and you might be wondering, what is that?
Socket preservation is a procedure we will sometimes recommend when you are having a tooth extracted. The bones that hold your teeth require frequent use to maintain their size and shape, otherwise they start to recede as they are no longer needed.
When a tooth is extracted, it leaves behind a hole (or “socket”) in the alveolar ridge bone, making it vulnerable to shrinkage. In fact, some studies show that bone loss can be 50% in the first 12 months after extraction.
You may be wondering, “Why does bone loss matter if I don’t have a tooth there anyway?” Unfortunately, without teeth and adequate bone structure, several unwanted oral health problems may occur:
- Aesthetics: Without adequate bone structure and teeth, your smile starts to cave in in that area, causing undesirable aesthetic consequences. Your skin may begin to look shriveled over time and your smile will be unbalanced and unnatural.
- Alignment Issues: Your teeth are always moving, particularly into open spaces. A hole on one side of your smile can lead to a severe shift of your teeth over time, affecting your smile and subsequently requiring orthodontic treatment.
- Implant Complications: The damaged and recessed bone often ensures complications if you plan on getting a dental implant to replace the extracted tooth in the future.
This is where socket preservation comes in. Typically done at the end of your extraction procedure, we place bone-grafting material into the socket and a collagen membrane on top to encourage bone growth in the area. Because the procedure can be done at the same time as your extraction, no additional anesthesia or appointments are necessary.
If you are facing extraction, call us at Houma Office Phone Number 985-879-1972 to see if socket preservation is an option for you – it could save your smile!
Posted by
csaal
on
Apr 5th, 2017
9:01 am
Posted in
Blog, Bone Grafting, Tooth Extraction |
Comments Off on Preserving Your Jaw after Extraction: Socket Preservation
Why do we have wisdom teeth anyway?
 Wisdom teeth were once an extremely valuable asset to our ancestors. When a typical diet consisted of chewy plants and uncooked meat, third molars (wisdom teeth), which fit easily into our ancestors’ larger jaws, were absolutely necessary. Wisdom teeth were the evolutionary answer to the need for chewing power to combat excessive wear.
Wisdom teeth were once an extremely valuable asset to our ancestors. When a typical diet consisted of chewy plants and uncooked meat, third molars (wisdom teeth), which fit easily into our ancestors’ larger jaws, were absolutely necessary. Wisdom teeth were the evolutionary answer to the need for chewing power to combat excessive wear.
Today, our diets are not as rough as those of our ancestors. With modern marvels like forks, spoons, and knives, as well as softer food, the need for wisdom teeth is virtually nonexistent. And yet, on average, about 65% of the human population is born with wisdom teeth which usually erupt between the ages 17 and 25.
Although wisdom teeth were incredibly advantageous for our ancestors, they pose a bit of a problem for the modern mouth. Humans have evolved to have smaller jaws, and so wisdom teeth are often either too big for the jaw or the jaws themselves are just too small. Either way, third molars crowd the mouth. Because of this lack of space, molars often grow sideways, only partially emerging from the gums, or actually get trapped inside the gums and jawbone.
These impacted wisdom teeth can be chronically contaminated with bacteria associated with infection, tooth decay, inflammation, and gum disease. And because they’re so far back in the mouth or trapped underneath gums, it’s difficult and sometimes impossible to keep them clean. Even when wisdom teeth come in fully, they are so far back in the mouth that it’s just too easy for food to get trapped, leading to plaque, cavities, and gum disease.
Although wisdom teeth were very important to our ancestors, nowadays, they pose a serious problem to oral health. Call Oral Facial Surgery Center to find out if your wisdom teeth are ready to come out!
Posted by
csaal
on
Mar 1st, 2017
9:00 am
Posted in
Blog, Wisdom Teeth |
Comments Off on Why do we have wisdom teeth anyway?